 Hormon dirençli veya radyoterapi sonrasý nüks eden lokal ileri prostat kanserinin radyoterapi ve hipertermi ile tedavisi
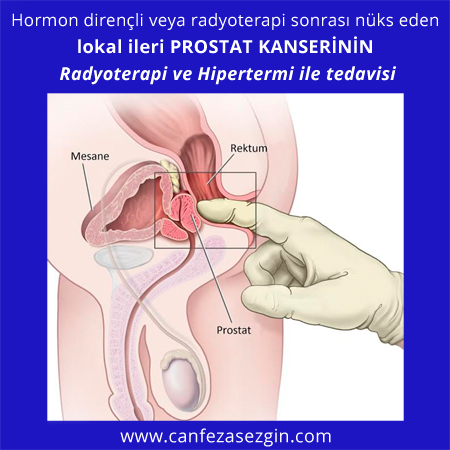
Hormon dirençli veya radyoterapi sonrasý nüks eden lokal ileri prostat kanserinin radyoterapi ve hipertermi ile tedavisi
Efficacy of irradiation and external hyperthermia in locally advanced, hormone-refractory or radiation recurrent prostate cancer: a preliminary report.
Int J Radiat Oncol Biol Phys. 2003 Nov 1;57(3):654-64.
Kalapurakal JA1, Pierce M, Chen A, Sathiaseelan V.
Author information
• 1Division of Radiation Oncology, Northwestern University, Robert H. Lurie Cancer Center, Chicago, IL 60611, USA. j-kalapurakal@northwestern.edu
Abstract
PURPOSE:
To present a preliminary report on the feasibility, efficacy, and toxicity of irradiation (RT) and hyperthermia (HT) in patients with locally advanced, hormone-refractory prostate cancer (LAHRPC) who may or may not have received prior RT.
METHODS AND MATERIALS:
Between 1997 and 2002, 13 consecutive patients with LAHRPC or RT-recurrent prostate cancer were treated with RT and HT on a Phase I-II protocol. Eight patients had RT-recurrent LAHRPC (Group A) and 5 had LAHRPC without prior RT (Group B). All patients had large and clinically symptomatic tumors. The median RT dose was 39.6 Gy and 66.6 Gy in Groups A and B, respectively. External deep HT was delivered using a BSD-2000 Sigma-60 applicator. The median number of HT treatments was 8 in group A and 10 in group B.
RESULTS:
The median follow-up was 14 and 13 months for Groups A and B, respectively. All patients achieved a complete or partial response (CR/PR) and complete palliation of symptoms. Eleven patients had follow-up CT scans that demonstrated a CR in six and a PR in five. Two patients, who died of metastasis, did not have CT scans and had a PR on digital rectal examination. Two patients demonstrated a biochemical CR. The median duration of the CR/PR among Group A patients was 12 months after therapy. Three patients in Group A developed tumor recurrence at 9, 17, and 27 months after repeat RT to doses of 39.6, 36, and 50 Gy, respectively. At last follow-up, no Group B patient developed local recurrence. Grade 1-2 rectal bleeding was noted in 3 patients. RT and HT were generally well tolerated by all patients who had not previously undergone RT. Of the 8 patients who had, 6 (75%) tolerated retreatment well with minimal or no complications. Two patients in the repeat RT group had severe complications. One patient with lymphoma and factor XI deficiency developed Grade 4 hemorrhagic cystitis. Another previously irradiated patient developed a rectovesical fistula 4 months after retreatment, after disappearance of a large, invasive, and necrotic tumor.
CONCLUSION:
This preliminary report demonstrates the feasibility and efficacy of RT and HT in patients with LAHRPC, who may or may not have received prior RT. Presently, such patients who have undergone previous RT have no effective treatment options. RT and HT were generally well tolerated by patients who were not previously undergone RT. Of those who had been, most (6 of 8) tolerated retreatment well with minimal or no complications. The high-risk factors for treatment- and tumor regression-related side effects include the presence of large necrotic tumors, previous RT with a large dose/fraction, and the presence of bleeding disorders. Despite the size of these large tumors, RT and HT resulted in significant tumor shrinkage, rapid serum prostate-specific antigen decline, durable treatment responses, and durable palliation of symptoms. Additional clinical studies are warranted.